As anti-Israel protesters continue to demonstrate across college campuses and rage at the White House's stance on the war ...
Anti-Israel protests may cost Biden election, supporters, journalists warn
Patrick Mahomes gets invite to Royals spring training: ‘He’s welcome anytime’
Patrick Mahomes may be turning back the clock just a little bit.Before he became a three-time Super Bowl champion ...
‘Standing on a corner in Winslow, Arizona’ is one American community’s route to revival
Jackson Browne was a rising singer-songwriter in 1972 when he penned one of the most memorable lines in American ...
Philly sheriff slammed for allegedly losing guns, AI-generated news stories, thousands spent on mascot, DJs
Much like Dolton, Illinois self-declared "Super Mayor" Tiffany Henyard, Philadelphia Sheriff Rochelle Bilal has been slammed with allegations of ...
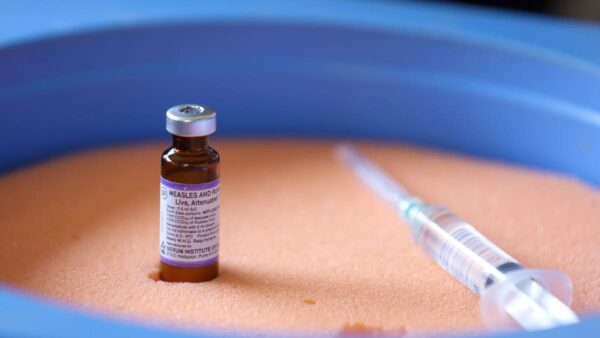
Measles confirmed in West Virginia in first case since 2009
A West Virginia hospital has confirmed the first known case of measles in the state since 2009, health officials said Monday. The […]
Chicago police release images of suspect wanted in shooting death of Officer Luis Huesca
Police in Chicago shared surveillance images of a suspect in connection to the murder of Officer Luis Huesca early Sunday morning as […]
AI could predict whether cancer treatments will work, experts say
A chemotherapy alternative called immunotherapy is showing promise in treating cancer — and a new artificial intelligence tool could help ensure that […]
Ex-NFL star against rookie QBs being thrown ‘into the fire’ as Caleb Williams likely to go No 1 to Bears
The Chicago Bears made the move to trade Justin Fields earlier in the offseason, which signaled they were likely ...
‘American Idol’ alum Mandisa death at 47 follows life of struggles, faith, inspiration
The death of "American Idol" alum Mandisa has left family, friends and fans devastated as an investigation is underway.Authorities ...
Slain Chicago police officer had gun, car stolen during attack: reports
The Chicago police officer who was shot and killed early Sunday morning while driving home from work had his ...
WNBA star Angel Reese: ‘Protect young women in sports’
Angel Reese, the former LSU national champion who was a top selection in the WNBA Draft last week, put ...
Chicago City Council approves $70M for migrant care despite voter backlash
The Chicago City Council on Friday green-lit an extra $70 million for the care of illegal immigrants in the Windy City despite […]
Yoko Ono to be awarded Edward MacDowell Medal for lifetime achievement
One of the country’s leading artist residency programs, MacDowell, has awarded a lifetime achievement prize to Yoko Ono. The groundbreaking artist, filmmaker […]
Female University of Chicago student disarms masked man who tried to rob her on walk home from class: report
A female University of Chicago student reportedly disarmed a robbery suspect who approached her on the sidewalk and demanded her phone as […]
Anti-Israel protests may cost Biden election, supporters, journalists warn
As anti-Israel protesters continue to demonstrate across college campuses and rage at the White House’s stance on the war in Gaza, more […]
Patrick Mahomes gets invite to Royals spring training: ‘He’s welcome anytime’
Patrick Mahomes may be turning back the clock just a little bit. Before he became a three-time Super Bowl champion and put […]
‘Standing on a corner in Winslow, Arizona’ is one American community’s route to revival
Jackson Browne was a rising singer-songwriter in 1972 when he penned one of the most memorable lines in American music history. “Well […]
Philly sheriff slammed for allegedly losing guns, AI-generated news stories, thousands spent on mascot, DJs
Much like Dolton, Illinois self-declared “Super Mayor” Tiffany Henyard, Philadelphia Sheriff Rochelle Bilal has been slammed with allegations of wild offenses ranging […]